Patient-centred radiology in New Zealand focuses on ensuring healthcare aligns with patient needs, preferences, and values. This approach integrates clear communication, respect for cultural practices, and equitable access to imaging services. Key initiatives include removing co-payments for community-referred radiology and prioritising patient involvement in care decisions. By July 2026, a nationwide programme will streamline access to X-rays, CT scans, and ultrasounds, improving both wait times and overall care quality. With a strong emphasis on compassion and inclusivity, radiology services in NZ aim to provide not just accurate diagnoses but also a supportive and respectful experience for all patients.
What Is Patient-Centred Radiology?
Patient-centred radiology focuses on more than just diagnosing and treating illnesses. It embraces a bio-psycho-social model, giving equal weight to physical, psychological, and social factors. This approach means radiologists consider not only the technical aspects of their work but also the patient’s experience, concerns, and personal context.
As William Osler wisely said, "It is much more important to know what sort of patient has a disease than what sort of disease a patient has".
In New Zealand, this philosophy is reflected in initiatives like the national community‐referred radiology programme, set to be fully implemented by July 2026. This programme aims to eliminate co‐payments, ensuring fair access to radiology services for all. Here’s how this approach translates into everyday practice.
Core Elements of Patient-Centred Care
Patient-centred radiology is built on four pillars: empathy, clear communication, respect for patient preferences, and shared decision-making.
Empathy involves more than technical skill. Studies show that when patients feel their healthcare provider understands their feelings, they communicate their symptoms more accurately, resulting in better diagnoses.
Clear communication is especially crucial in diverse regions like Auckland. For example, professional interpreters should be used during complex procedures, such as contrast-enhanced CT scans, instead of relying on family members, whose emotional involvement might affect accuracy. Radiographers should also use plain language and an approachable tone, steering clear of any condescension, to ensure patients feel respected and understood.
Shared decision-making gives patients an active role in their care. This can involve bedside handovers or tools like the Patient Specific Function Scale to align treatment with patient priorities. For Māori and Pacific patients, involving whānau (family) in the process offers emotional and spiritual support – taha hinengaro and taha wairua – that significantly enhances outcomes.
These practices not only improve patient care but also foster better outcomes for healthcare providers.
Benefits for Patients and Providers
Patient-centred radiology delivers clear advantages for everyone involved. Patients often feel less anxious when procedures are explained thoroughly, which leads to better cooperation and more accurate imaging results. Feeling respected and heard also increases their willingness to follow treatment plans and attend follow-up appointments.
For healthcare providers, this approach builds trust within the community and improves job satisfaction. Radiographers find that taking the time to connect with patients – despite the pressures of a busy schedule – makes their work smoother, as relaxed patients often require fewer repeat scans. Moving from "cultural competence" (understanding different backgrounds) to "cultural safety" (ensuring patients feel genuinely safe and respected) involves continuous self-reflection on power dynamics, leading to care that truly meets diverse needs.
A standout example is the Nelson Marlborough DHB, which uses co-design and experience-based surveys, rather than generic questionnaires, to directly involve patients in improving radiology services.
sbb-itb-16a0ccc
Respecting Different Cultures in New Zealand Radiology
In New Zealand’s radiology sector, cultural safety goes beyond simply acknowledging diverse backgrounds. It challenges healthcare providers to reflect on power dynamics and personal biases, ensuring patients feel genuinely respected and safe. This is particularly crucial in Auckland, the nation’s most diverse region, where te reo Māori is the second most spoken language after English. Below, we explore how Māori values are integrated into radiology practices and how equitable access to care is being prioritised.
Incorporating Māori Values
Radiology providers across New Zealand are embracing the principles of Te Tiriti o Waitangi – partnership, participation, and protection – to uphold the dignity and respect of Māori patients. For instance, Beyond Radiology has woven these principles into its core values, fostering a welcoming and inclusive environment for all patients.
Practical steps are central to this integration. In January 2026, Pinnacle Practices introduced the "Tikanga in practice" resource. This includes wall posters for consultation rooms and flipbooks for staff, offering clear guidance on behaviours that enhance mana. These range from greeting patients with "Kia Ora" and correctly pronouncing names to respecting tapu (sacred) and noa (unrestricted) concepts, such as using specific white pillows for the head and avoiding sitting on clinical surfaces.
Staff are also trained to support karakia (prayer) before, during, or after consultations – particularly before major procedures or when delivering difficult news. Radiographers are encouraged to securely tape taonga to the patient’s body, or, if removal is necessary, ensure the patient or their whānau handles it first for safekeeping.
While cultural alignment is essential, structural changes are also driving fairer access for all New Zealanders.
Ensuring Fair Access to Healthcare
To address financial barriers, the government has committed NZ$30 million annually to a community-referred radiology programme. This initiative, set to be fully operational by July 2026, removes co-payments for X-rays, CT scans, and ultrasounds that meet national clinical criteria. By doing so, it ensures equitable access regardless of location.
Health New Zealand is also rolling out Enhanced Access services, which use health navigators to assist underserved groups – such as Māori, Pacific peoples, and rural communities – in accessing diagnostic imaging. General Practitioners, Urgent Care Doctors, and Nurse Practitioners now have the authority to directly refer patients, enabling faster diagnoses and treatment plans. Additionally, efforts to recruit healthcare teams that reflect New Zealand’s cultural diversity are helping to bridge language gaps. This is particularly important given that approximately 25,000 New Zealanders rely on New Zealand Sign Language.
How to Access Radiology Services in New Zealand
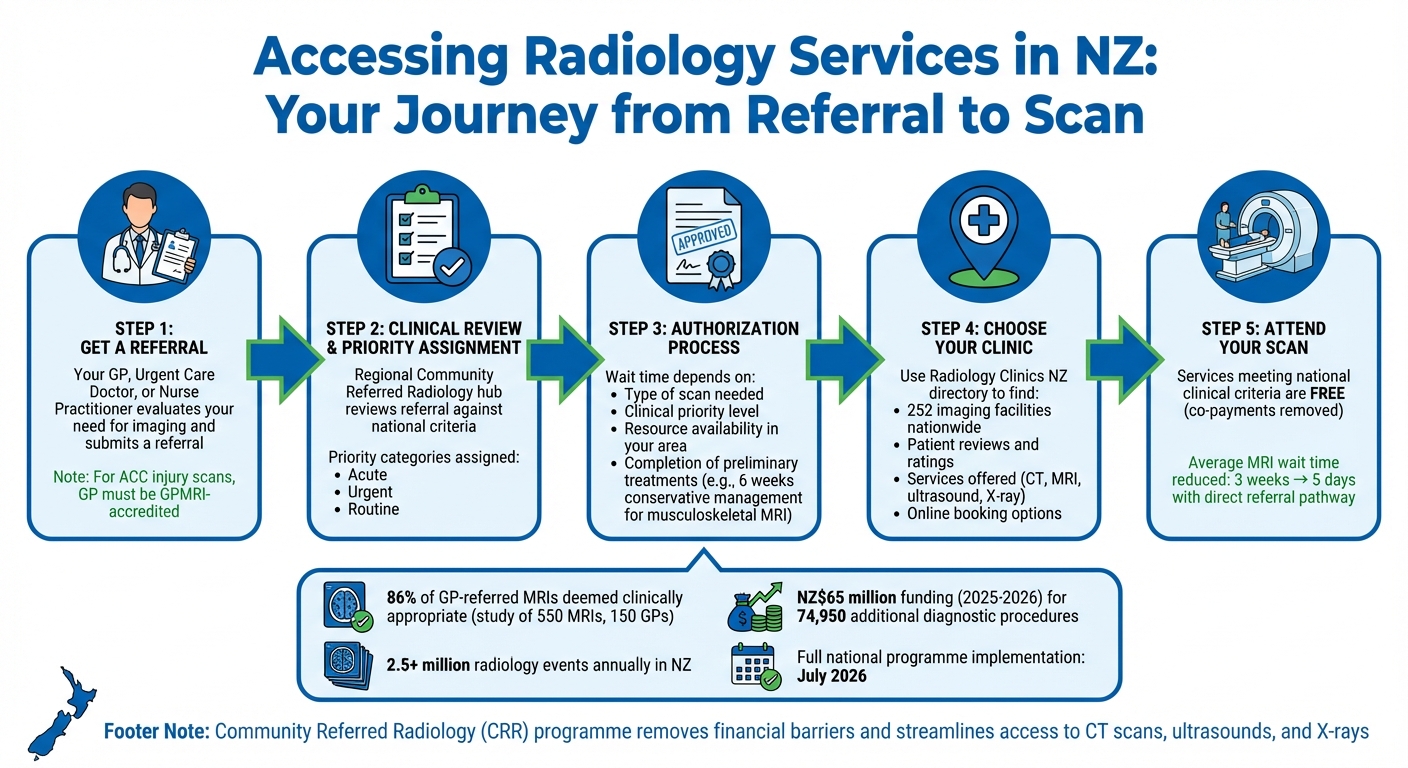
How to Access Radiology Services in New Zealand: Referral to Scan Process
Accessing radiology services in New Zealand begins with a referral from your GP, Urgent Care Doctor, or Nurse Practitioner. This ensures imaging resources are used effectively and helps deliver timely and accurate diagnoses.
Referral and Priority Categories
Your GP or another authorised healthcare provider will evaluate your need for imaging. Once they submit a referral, clinical staff at a Regional Community Referred Radiology hub review it against national criteria, assigning it a priority category: acute, urgent, or routine.
For injury-related scans funded by ACC, the process has specific requirements. Your GP must be accredited under the GP Referred MRI (GPMRI) programme to directly refer for MRIs of the knee, lumbar spine, or cervical spine. A study involving 550 MRIs ordered by 150 GPs found that 86% of these referrals were deemed clinically appropriate. If your injury is more complex or involves other areas, your GP may refer you to a General Practitioner with a Special Interest (GPSI), who has advanced training and authority for musculoskeletal imaging referrals.
The Community Referred Radiology (CRR) programme, which is expected to be fully implemented by July 2026, will allow for direct community referrals for imaging such as CT scans, ultrasounds, and X-rays without needing a hospital specialist’s assessment. This programme has already streamlined MRI referrals, cutting wait times from three weeks to an average of five days.
Dr Stephen Kara, lead author of the MRI referral study, highlighted: "The direct referral pathway significantly reduces wait times from referral to MRI report, down from three weeks to an average of five days, creating a much better patient experience".
Managing Wait Times and Authorisation
Several factors determine how quickly you can access imaging after your referral. These include the type of scan needed, your clinical priority, the availability of resources in your area, and whether you’ve completed any required preliminary treatments. For example, many musculoskeletal imaging guidelines require six weeks of conservative management before an MRI can be authorised.
To ensure your referral is processed smoothly, your referrer should include a detailed clinical history. This helps triage staff prioritise your case more accurately. If your symptoms worsen, you can contact your referrer to request a priority upgrade. For ACC-funded scans, it’s important to confirm that your claim has been accepted before your referral is processed.
New Zealand is making significant investments to improve access to radiology services. Health New Zealand has allocated NZ$65 million for the 2025–2026 period to fund an additional 74,950 diagnostic procedures, aiming to tackle backlogs and reduce wait times nationwide. With over 2.5 million radiology events taking place annually, this funding reflects a strong commitment to improving accessibility. Services meeting national clinical criteria are now free for patients, as previous co-payments have been removed to eliminate financial barriers.
Finding Patient-Focused Radiology Clinics
Choosing the right radiology clinic is an essential step in ensuring a smooth, patient-centred care experience. Once you have your referral, it’s important to select a clinic that prioritises your comfort and overall wellbeing. The Radiology Clinics NZ directory is a helpful resource, offering details on 252 radiology imaging options across New Zealand. You can refine your search by facility type, such as Ultrasound Clinics, Accident & Emergency Centres, or Hospitals.
Using Radiology Clinics NZ Directory
The directory allows you to search for clinics by location and the type of scan you need – whether it’s CT, MRI, ultrasound, or X‑ray. Each clinic profile includes essential details like address, operating hours, and available services (e.g., CT Colonography, Pregnancy Ultrasound, or MRI). For easy decision-making, the platform highlights "Top rated listings", complete with star ratings ranging from 0.0 to 5.0. For instance, Pacific Radiology – Porirua and Greenlane Clinical Centre both hold a perfect 5.0-star rating, reflecting excellent patient feedback.
The "Explore Radiology Practices" section offers patient reviews, which provide valuable insights into service quality and staff friendliness. One patient, Sharyne Dallas, shared her positive experience at Pacific Radiology – Porirua:
"She was so lovely funny efficient and l felt at ease with her".
Similarly, Linda Wong praised the Greenlane Clinical Centre, saying:
"Staff at the Greenlane Clinical Centre Radiology Dept delivered excellent customer service in the communication lead up and on the day care".
This directory simplifies the process of finding trusted clinics, aligning with a patient-centred care approach. Use it to explore reviews and ensure the clinic matches your expectations for quality care.
Assessing Clinic Services and Reviews
When reading patient reviews, pay close attention to comments about communication and staff empathy. Clinics that are described as "compassionate", "calm", or "professional" often stand out for their patient-focused care, especially during procedures that can be stressful [20,21]. Reviews mentioning staff who help patients feel "at ease" or provide clear explanations are strong indicators of high-quality service.
It’s also important to note recurring criticisms. Common complaints include long wait times for appointments, extended phone hold periods, or unprofessional behaviour from reception staff. For example, Wayne Moore voiced his frustration:
"Had an appointment today at 1.30pm as usual had to wait 25 minutes I think this is unacceptable especially when my time is just as valuable".
To avoid such issues, look for clinics with online booking systems, which can save time and reduce phone delays. Additionally, check recent reviews to get a sense of current wait times. Clinics that invest in advanced technology and employ subspecialist radiologists are often better equipped to deliver both high-quality care and a positive patient experience [20,22]. These tips will help you make an informed decision as you continue to evaluate patient safety and overall care standards in the next section.
Best Practices for Patient Safety and Experience
Safe and Comfortable Imaging Procedures
Radiology clinics in New Zealand follow strict safety protocols to ensure patient protection during imaging exams. One key guideline is the ALARA principle ("As Low As Reasonably Achievable"), which drives clinics to use advanced digital radiography (DR) technology. This approach minimises radiation exposure while maintaining high-quality diagnostic images.
For MRI safety, clinics implement a thorough three-stage screening process. This includes checks during booking, a written questionnaire upon arrival, and a verbal confirmation before the scan. These steps are crucial, especially for the 10% to 20% of MRI patients who have implanted medical devices, as these devices require careful evaluation to avoid complications. It’s essential for patients to inform staff about any implants, devices, or past surgeries during these screenings.
Beyond technical safeguards, clinics prioritise patient comfort and individual needs. In line with New Zealand’s focus on patient-centred care, communication is adapted to accommodate linguistic and cultural preferences, ensuring fairness across diverse populations, including Māori. For patients with specific cultural or religious requirements, clinics can arrange for female radiographers to conduct sensitive procedures. Additionally, including whānau (family) during imaging sessions offers emotional support, which is particularly valued in Māori culture, as long as radiation safety measures are upheld.
Leveraging Patient Feedback
Safety protocols are just one piece of the puzzle – radiology clinics also rely on patient feedback to improve care. Feedback often highlights communication issues that could lead to errors, such as patients misunderstanding instructions or not accurately describing their symptoms. Researchers Nica Abrasado and Sibusiso Mdletshe emphasise the importance of rapport in patient experiences:
"Patients tend to appreciate their experience within the healthcare system based on the established reciprocal, relational rapport more so than the technical aspects of acquiring diagnostic acceptable images".
In 2015, the Nelson Marlborough District Health Board (NMDHB) initiated a Radiology Service Improvement Initiative as part of a nationwide effort. Spearheaded by Dr Thomas Bryant, Clinical Head of Department, the project introduced "experience-based surveys" and a co-design model to go beyond standard surveys. Dr Bryant explained:
"We hoped that [experience-based surveys] would give us a clearer picture of how we could change processes in collaboration with our patients".
Leading radiology providers like Pacific Radiology and Auckland Radiology Group now incorporate digital feedback forms on their websites. These tools collect real-time patient insights, enabling clinics to refine their processes in direct partnership with patients. Patients are encouraged to use these platforms to share concerns, as this feedback is vital for ongoing improvements in quality and care.
Conclusion: Empowering Patients Through Patient-Centred Radiology
Patient-centred radiology is reshaping diagnostic imaging in New Zealand by putting the focus on the patient, not just the condition. This approach encourages patients to actively participate in their healthcare, working in partnership with professionals instead of being passive recipients. The benefits are clear: more accurate diagnoses, reduced anxiety, and care that respects cultural values – especially for Māori, where spiritual and emotional needs are honoured through whānau involvement and alignment with Te Tiriti o Waitangi principles. Thanks to Health New Zealand’s $30 million annual funding for community-referred radiology and the removal of co-payments for services that meet national clinical criteria, financial hurdles are no longer a barrier to accessing essential imaging services.
These improvements are being rolled out nationwide. By July 2026, a fully implemented national programme will ensure timely access to CT scans, ultrasounds, and X-rays across all regions. General practitioners will have the ability to refer patients directly for imaging, and community-based care will be enhanced with digital tools for self-management, providing quicker answers and better outcomes.
This patient-first approach reflects a strong commitment to care that considers individual needs at every stage of the radiology process. With these advancements in place, choosing the right clinic becomes even more important. Radiology Clinics NZ offers a searchable directory to help you compare clinics by location, read patient reviews, and find facilities offering tailored services – like online booking, multilingual staff, or gender-specific radiographers to meet cultural or religious preferences. By selecting clinics that prioritise clear communication, cultural respect, and whānau involvement, you’re not just receiving medical care – you’re engaging with a healthcare system built around your wellbeing.
FAQs
What should I ask before a scan to feel more in control?
To feel more prepared and at ease before a scan, consider discussing the following with your healthcare provider or radiology team:
- Preparations required: Find out if you need to fast, adjust medications, or follow any specific instructions before the scan.
- What to expect during the scan: Ask about the process, including any sensations you might feel or noises from the equipment.
- Concerns about implants or devices: If you have metallic implants or medical devices, check if they could affect the scan.
- Duration of the procedure: Understand how long the scan is expected to take.
These discussions can help you feel more informed and ready, both mentally and physically, for the procedure.
Can I bring whānau and request cultural support during imaging?
Yes, you can bring whānau and request support that aligns with your cultural needs during imaging procedures. Healthcare providers in New Zealand are encouraged to create an environment that respects Māori values, including the presence of whānau for support. This reflects the principles of patient-centred care, ensuring respect and inclusivity in healthcare settings.
How do I check if my scan will be free and how long I might wait?
Contact your radiology provider directly to check if your scan will be free and to get an idea of the wait times. The cost can vary depending on factors like ACC cover, private insurance, or if you’re paying upfront. Wait times often depend on the facility and current demand, though steps are being taken to minimise delays. Your provider can also guide you on payment options and whether a referral is needed.

Leave a Reply